You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Dental hypersensitivity (DH) affects approximately 40 million Americans at least once during their lifetimes.1 The problem has various terms, such as tooth sensitivity, cervical root sensitivity, or simply “sensitivity,” and can have many etiologies. DH may occur from root surface denudation of the cementum and/or dentin, enamel loss from erosion, abrasion, abfraction, and root surface exposure due to gingival recession or periodontal therapy.2,3 DH is considered multifactorial, with layers of each etiology helping to exacerbate the problem. The condition displays an exaggerated pain response to normal tactile contact, temperature variation, and osmotic, evaporative, or chemical stimuli. The classic description of DH is a dental history of sharp, acute cold sensitivity.4 Osmotic stimuli, such as bleaching and evaporation, can also elicit a reaction.
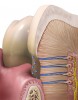
Usually, these patients report the sensitivity occurring after a recent hygiene appointment. This is common because the occluded dentinal tubules are uncovered during a prophylaxis.5-8 The most reported and accepted explanation was first described by Brännström.9-12 He postulated that inward or outward movement of fluid within the tubules stimulates the odontoblasts and associated nerve fibers, resulting in a painful nerve response as fluid moves rapidly in and out of the tubule (Figure 1). Some people are more sensitive to these changes because the configuration, number, and diameter of open tubules are responsible for the response severity. In a study in the Journal of the American Dental Association, Purk et al revealed that cervical dentin is 3.6 times more permeable than occlusal dentin in young adults.13,14
Causes
The most frequent causes of dentinal sensitivity are related to the following:
Brushing with excessive pressure and with hard toothbrush bristles. Hard, long-term brushing can erode the enamel and cause dentinal exposure. It can also lead to gingival recession, exposing the cementum, which is easily eroded to reveal the dentinal tubules; the cemento-enamel junction has a higher number of tubules.15-18
Gingival recession with various etiologies will expose the dentin and increase sensitivity.19-21
Periodontal disease can cause the destruction of the supporting periodontal apparatus, exposing cementum and dentin, which increases the number of exposed tubules. The increasing root exposure will raise the patient’s sensitivity.15
Although debated by some researchers, bruxing or parafunctional habits may cause abfractions and expose dentin. Others suggest that the lateral forces due to parafuction and bruxing cause loss of crestal bone, leading to recession and dentinal exposure.22-24
Tooth whitening products increase the osmotic gradient and remove tubal occlusions.25-27
Abrasive toothpastes, such as baking soda, will expose dentinal tubules.22,28,29
Research has shown that age can contribute to DH.22
Plaque buildup and poor oral hygiene, with the increase in acid-producing plaque, will cause dentinal erosion.30
Mouthwashes and mouthrinses have an acidic pH and can dissolve tooth structure, increasing dentinal exposure.19
Acidic food and beverages, with the pH of some juices and soda reaching as low as 4, have been shown to dissolve the organic layer of dentin. This uncovers previously blocked tubules and removes dentinal tissues.22
Recent dental treatment, such as periodontal surgery, scaling and root planing, operative procedure, and prophylaxis, can cause an increased exposure of dentinal tubules and elicit a greater sensitivity to temperature, sweets, and other factors.19-21
Diagnosis
The practitioner must perform a thorough evaluation of the patient’s perceived sensitivity because there can be several differential diagnoses. Taking an accurate and complete dental history is essential. A clinical examination, which should include an assessment of current radiographs, is necessary to rule out a carious lesion, cracked tooth syndrome, chipped teeth, sinusitis, hypoplastic enamel, fractured restorations, improperly insulated metallic restorations, or traumatic occlusion yielding reversal pulpitis. These are some of the conditions that can be confused with DH.28
Professional, Topically Applied Therapies
In a true case of DH, the treatment course centers on the ability to occlude or seal the tubules and reduce the movement of fluid into and out of the tooth and, therefore, block the excitation of pulpal nerve fibers. The blockage of neural transmissions can also be achieved by the use of potassium salts.31 The most popular agents in desensitizers are: ions, salts, protein-amino acid precipitates, and resins.32 The most used tubule-occluding or sealing materials include fluoride, amorphous calcium and phosphate, sodium phosphates, potassium nitrate, resin bonding agents, oxalate-containing resins, and glutaraldehydes.33-43 Although often effective, glutaraldehydes have recently come under scrutiny due to their cellular-cidal nature and the concerns regarding the environmental exposure health effects.44-46
Fluoride is the most prescribed and most used agent to reduce DH. It is available in various states and concentrations in either over-the-counter (OTC) formulations or prescription and professionally applied doses.47 The substance can be applied as a toothpaste, rinse, gel (tray), or varnish. Sodium fluoride or calcium fluoride are the most popular forms. Fluoride is also combined with other compounds or used as an adjunct to a remineralizing therapy, such as MI Paste™ (GC America, www.gcamerica.com), which contains calcium.48 These treatments have been shown to significantly reduce DH but longevity is linked to concentration and application method.
Resins have shown a good clinical history with significant reductions in DH. The dentist should not have support staff apply bonding resins because use of these materials is very technique sensitive and require moisture control to achieve optimal results. Clinical studies using bonded resins have shown that reduction in sensitivity lasts as long as 1 year.46,49-54
Oxalic acid-containing desensitizing agents react with ionized calcium within the dentinal tubule to form insoluble calcium oxalate crystals. An example is PAIN-FREE™ Desensitizer (Parkell, www.parkell.com), which also contains a poly(methyl methacrylate)-co-p-styrenesulfonic acid polymer (90% poly[methyl methacrylate] and 10% p-styrene sulfonic acid) that forms a tri-polymer sealing. This creates a surface film over the dentin. The oxalate precipitates below the polymer film in the tubule. This surface film also gives the precipitation time to occur deep in the tubule. Clinical studies by both Zhang et al and Morris et al have shown the clinical efficacy of this desensitizer.36,37,41
Adjunctive Home Therapies
These self-applied OTC treatments are cost effective for the patient. Because these products have shown mixed results, they should be viewed as adjuncts to professional therapies.20 To achieve the best results in treating DH, the dentist should educate the patient about the condition’s causes and compounding factors. With the patient, the clinician should review proper oral hygiene instruction, discuss modifying aggressive brushing habits, and verify that the patient is using low pressure when brushing to ensure a decrease in bristle deflection. Also, ask about the dentifrice that the patient is using and recommend a clinically acceptable low-abrasive toothpaste, such as Crest® ProHealth (Procter and Gamble, www.pg.com) or Sensodyne® (GlaxoSmithKline, www.gsk.com). These dentifrices, which are regulated by the Food and Drug Administration, have clinically verified tubule-blocking properties, such as potassium nitrate and low abrasion. In combination with a gentle brushing technique, these measures can yield a reduction in DH.28,29,33-35
Fluoride mouthrinse and prescription fluoride toothpaste, such as Durphat® (Colgate-Palmolive, www.colgate.com), can be used if adequate results are not noted after modifying the patient’s brushing technique and ensuring the use of a low-abrasive toothpaste.
The combination of professionally applied dentinal occluding and sealing agents along with a modified home oral care regimen will maximize the reduction in dentin sensitivity.
Click here to view a case study.
Conclusion
Understanding the etiology is important for proper diagnosis and treatment of DH. With the numerous choices in materials available, the general practitioner should select the treatment that has demonstrated proven clinical effectiveness. An important consideration is the application time and simplified technique that would enable a support staff member, such as a dental hygienist, to easily apply the treatment during the routine hygiene visit with no need for direct supervision or anesthetic injection. When choosing a dentin desensitizer, a clinician should base the selection on an agent that has clinically shown immediate reduction in perceived sensitivity.
Disclosure
Dr. Anderson received an honorarium from AEGIS Publications, LLC.
References
1. Scherman A, Jacobsen PL. Managing dentin hypersensitivity: what treatment to recommend to patients. J Am Dent Assoc. 1992;123(4):57-61.
2. Dababneh RH, Khouri AT, Addy M. Dentine hypersensitivity—an enigma? A review of terminology, epidemiology, mechanisms, aetiology and management. Br Dent J. 1999;187(11):606-611.
3. Camps J, Pashley D. In vivo sensitivity of human root dentin to air blast and scratching. J Periodontol. 2003;74(11):1589-1594.
4. Holland GR, Narhi MN, Addy M, et al. Guidelines for the design and conduct of clinical trials on dentine hypersensitivity. J Clin Periodontol. 1997;24(11):808-813.
5. Pamir T, Dalgar H, Onal B. Clinical evaluation of three desensitizing agents in relieving dentin hypersensitivity. Oper Dent. 2007;32(6):544-548.
6. Ritter AV, de L Dias W, Miguez P, et al. Treating cervical dentin hypersensitivity with fluoride varnish: a randomized clinical study. J Am Dent Assoc. 2006;137(7):1013-1020.
7. Burke FJ, Malik R, McHugh S, et al. Treatment of dentinal hypersensitivity using a dentine bonding system. Int Dent J. 2000;50(5):283-288.
8. Kielbassa AM. Dentin hypersensitivity: simple steps for everyday diagnosis and management. Int Dent J. 2002;52(5 suppl 1):394-396.
9. Brännström MA. Dentinal and pulpal response: II. Application of an air stream to exposed dentine. Acta Odont Scand. 1960;18:17-28.
10. Brännström MA. The elicitation of pain in the human dentin and pulp by chemical stimulation. Arch Oral Biol. 1962;7:59.
11. Brännström M. Sensitivity of dentine. Oral Surg Oral Med Oral Pathol 1966;21(4):517-526.
12. Brännström M. The hydrodynamic theory of dentinal pain: sensation in preparations, caries, and the dentinal crack syndrome. J Endod. 1986;12(10):453-457.
13. Purk JH, Healy M, Dusevich V, et al. In vitro microtensile bond strength of four adhesives tested at the gingival and pulpal walls of Class II restorations. J Am Dent Assoc. 2006;137(10):1414-1418.
14. Purk J, Dusevich V, Glaros A, et al. In vivo versus in vitro microtensile bond strength of axial versus gingival cavity preparation walls in Class II resin-based composite restorations. J Am Dent Assoc. 2004;135(2):185-193.
15. Bánóczy J. Dentine hypersensitivity-general practice considerations for successful management. Int Dent J. 2002;52(suppl):366.
16. Cox CF. Etiology and treatment of root hypersensitivity. Am J Dent. 1994;7(5):266-270.
17. Addy M. Dentin hypersensitivity: definition, prevalence, distribution aetiology. In: Addy M, Embery G, Edgar WM, et al; eds. Tooth Wear and Sensitivity Clinical Advances in Restorative Dentistry. London, United Kingdom: Martin Dunitz; 2000:239-248.
18. Addy M. Dentine hypersensitivity: new perspective on an old problem. Int Dent J. 2002;52:367-375.
19. Barrow SL. Dentin hypersensitivity—an overview. Dimens Dent Hyg. 2006;4(6):28,30.
20. Orchardson R, Gangarosa LP Sr, Holland GR, et al. Dentine hypersensitivity—into the 21st century. Arch Oral Biol. 1994;39(suppl):S113-S119.
21. Gysi A. An attempt to explain the sensitiveness of dentin. Br J Dent Sci. 1900;43:865-868.
22. Abrahamsen TC, The worn dentition—pathognomonic patterns of abrasion and erosion. Int Dent J. 2005;55(4 suppl 1);268-276.
23. Scheutzel P. Etiology of dentin erosion—intrinsic factors. Eur J Oral Sci. 1996;104:178-190.
24. Tilliss TS, Keating JG. Understanding and managing dentin hypersensitivity. J Dent Hyg. 2002;76(4):296-313.
25. Leonard RH Jr, Haywood VB, Phillips C. Risk factors for developing tooth sensitivity and gingival irritation associated with nightguard bleaching. Quintessence Int. 1997;28(8):527-534.
26. Nathanson D. Vital tooth bleaching: sensitivity and pulpal considerations. J Am Dent Assoc. 1997;128(suppl):S41-S44.
27. Gerlach RW, Gibb RD, Sagel PA. A randomized clinical trial comparing a novel 5.3% hydrogen peroxide whitening strip to 10%, 15%, and 10% carbamide peroxide tray-based bleaching systems. Compend Contin Educ Dent Suppl. 2000;(29):S22-S28.
28. Silverman G, Berman E, Hanna CB, et al. Assessing the efficacy of three dentrifices in the treatment of dentinal hypersensitivity. J Am Dent Assoc. 1996;127(2):191-201.
29. Recommendations for evaluating agents for the reduction of dentinal hypersensitivity. Ad Hoc Advisory Committee on Dentinal Hypersensitivity, Council on Dental Therapeutics. J Am Dent Assoc. 1986;112(5):709-710.
30. Bissada NF. Symptomatology and clinical features of hypersensitive teeth. Arch Oral Biol. 1994;39(suppl):S31-S32.
31. Haywood VB. Dentin hypersensitivity: bleaching and restorative considerations for successful management. Int Dent J. 2002;52(5 suppl 1):376-384.
32. Jacobsen PL, Bruce G. Clinical dentin hypersensitivity: understanding the causes and prescribing a treatment. J Contemp Dent Pract. 2001;2(1):1-12.
33. Kern DA, McQuade MJ, Scheidt MJ, et al. Effectiveness of sodium fluoride on tooth hypersensitivity with and without iontophoresis. J Periodontol. 1989:60(7):386-389.
34. Pearce NX, Addy M, Newcombe RG. Dentine hypersensitivity: a clinical trial to compare 2 strontium desensitizing toothpastes with a conventional fluoride toothpaste. J Periodontol. 1994:65(2):113-119.
35. Haywood VB, Caughman WF, Frazier KB, et al. Tray delivery of potassium nitrate-fluoride to reduce bleaching sensitivity. Quintessence Int. 2001;32(2):105-109.
36. Zhang Y, Agee K, Pashley DH, et al. The effects of Pain-Free Desensitizer on dentine permeability and tubule occlusion over time, in vitro. J Clin Periodontol. 1998;25(11 pt 1):884-891.
37. Morris MF, Davis RD, Richardson BW. Clinical efficacy of two dentin desensitizing agents. Am J Dent. 1999;12(2):72-76.
38. Pillon FL, Romani IG, Schmidt ER. Effect of a 3% potassium oxalate topical application on dentinal hypersensitivity after subgingival scaling and root planing. J Periodontol. 2004;75(11):1461-1464.
39. Tay FR, Pashley DH, Mak YF, et al. Integrating oxalate desensitizers with total-etch two-step adhesive. J Dent Res. 2003;82(9):703-707.
40. Pashley EL, Tao L, Pashley DH. Effects of oxalate on dentin bonding. Am J Dent. 1993;6(3):116-118.
41. Erdemir U, Yildiz E, Kilic I, et al. The efficacy of three desensitizing agents used to treat dentin hypersensitivity. J Am Dent Assoc. 2010;141(3):285-296.
42. Muzzin KB, Johnson R. Effects of potassium oxalate on dentin hypersensitivity in vivo. J Periodontol. 1989;60(3):151-158.
43. Gillam DG, Newman HN, Davies EH, et al. Clinical evaluation of ferric oxalate in relieving dentine hypersensitivity. J Oral Rehabil. 2004;31(3):245-250.
44. Lewis B. The obsolescence of formocresol. J Calif Dent Assoc. 2010;38(2):102-107.
45. Dondi dall’Orologio G, Lorenzi R, Anselmi M, et al. Dentin desensitizing effects of Gluma Alternate, Health-Dent Desensitizer and Scotchbond Multi-Purpose. Am J Dent. 1999;12(3):103-106.
46. Kakaboura A, Rahiotis C, Thomaidis S, et al. Clinical effectiveness of two agents on the treatment of tooth cervical hypersensitivity. Am J Dent. 2005;18(4):291-295.
47. Kielbassa AM, Attin T, Hellwig E, et al. In vivo study on the effectiveness of a lacquer containing CaF2/NaF in treating dentine hypersensitivity. Clin Oral Investig. 1997;1(2):95-99.
48. Matis B, Cochran MA, Ekert GJ, et al. In vivo study of two carbimide peroxide gels with different desensitizing agents. Oper Dent. 2007;32(6):549-555.
49. Baysan A, Lynch E. Treatment of cervical sensitivity with a root sealant. Am J Dent. 2003;16(2):135-138.
50. Ferrari M, Cagidiaco MC, Kugel G, et al. Clinical evaluation of a one-bottle bonding system for desensitizing exposed roots. Am J Dent. 1999;12(5):243-249.
51. Duran I, Sengun A. The long-term effectiveness five current desensitizing products on cervical dentin sensitivity. J Oral Rehabil. 2004;31(4):351-356.
52. Prati C, Cervellati F, Sanasi V, et al. Treatment of cervical dentin hypersensitivity with resin adhesives: 4-week evaluation. Am J Dent. 2001;14(6):378-382.
53. Jain P, Reinhardt JW, Krell KV. Effect on dentin desensitizers and dentin bonding agents on dentin permeability. Am J Dent. 2000;13(1):21-27.
54. Swift EJ Jr, May KN Jr, Mitchell S. Clinical evaluation of Prime & Bond 2.1 for treating cervical dentin hypersensitivity. Am J Dent. 2001;14(1):13-16.